Problems We Focus On

STIs and HIV: Women and Children
Embark on a Path of Hope: Maternova's Lifesaving Solutions for Women and Children

Women's Reproductive Health
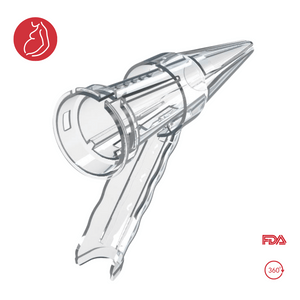
Experience the Cutting-Edge Bouquet Speculum:
Advancing Women's Reproductive Well-being.
Work with us

Humanitarian and Developmental Organizations
Maternova provides essential medical supplies for women and infants wherever your health centers and medical units need them. As a pre-approved vendor on the UN Global Marketplace, we supply trusted and tested medical devices and diagnostics that meet WHO criteria.

Ministries of Health
Maternova advises your ministers of health on medical devices and diagnostics that align with your public health objectives and strategies. We are prequalified as a vendor to the UN on the UN Global Marketplace and work closely with you to procure and distribute the most useful and cost-effective medical technology available to save the lives of women and babies.

Distributors
Maternova offers a well curated range of evidence-based medical technologies that expands and differentiates your offerings. We specialize in maternal, fetal, and child health innovation and work with you to make a clinical case to your network of hospitals and clinics.
Listen to our customers

Benefits of intravenous iron to treat anemia in pregnancy

A Point of Care Bilirubinometer Using Blood: BiliDx